 Claudication is pain caused by too little blood flow to muscles during exercise. Most often this pain occurs in the legs after walking at a certain pace and for a certain amount of time — depending on the severity of the condition.
Claudication is pain caused by too little blood flow to muscles during exercise. Most often this pain occurs in the legs after walking at a certain pace and for a certain amount of time — depending on the severity of the condition.
The condition is also called intermittent claudication because the pain usually isn’t constant. It begins during exercise and ends with rest. As claudication worsens, however, the pain may occur during rest.
Claudication is technically a symptom of disease, most often peripheral artery disease, a narrowing of arteries in the limbs that restricts blood flow.
Treatments focus on lowering the risks of vascular disease, reducing pain, increasing mobility and preventing damage to tissues.
Symptoms
Claudication refers to muscle pain due to lack of oxygen that’s triggered by activity and relieved by rest. Symptoms include the following:
- Pain, ache, discomfort or fatigue in muscles every time you use those muscles
- Pain in the calves, thighs, buttocks, hips or feet
- Less often, pain in shoulders, biceps and forearms
- Pain that gets better soon after resting
The pain may become more severe over time. You may even start to have pain at rest.
Signs or symptoms of peripheral artery disease, usually in more-advanced stages, include:
- Cool skin
- Severe, constant pain that progresses to numbness
- Skin discoloration
- Wounds that don’t heal
Causes
Claudication is most often a symptom of peripheral artery disease. The peripheral arteries are the large vessels that deliver blood to the network of vessels in your legs and arms.
Peripheral artery disease is damage to an artery that restricts the flow of blood in an arm or leg (a limb). When you’re at rest, the limited blood flow is generally still enough. When you’re active, however, the muscles aren’t getting enough oxygen and nutrients to work well and remain healthy.
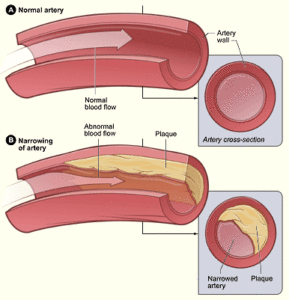
Damage to peripheral arteries is usually caused by atherosclerosis. This is the buildup of cholesterol and other fats, blood cells, and other cellular debris into abnormal structures (plaques) on the lining of an artery.
Plaques cause a narrowing and stiffening of the artery, limiting the flow of blood. If the plaques rupture, a blood clot can form, further reducing blood flow.
Risk factors
The risk factors for peripheral artery disease and claudication include the following:
- Smoking
- High cholesterol
- High blood pressure
- Obesity (a body mass index, or BMI, over 30)
- Diabetes
- Chronic kidney disease
- Age older than 70 years
- Age older than 50 years if you also smoke or have diabetes
- A family history of atherosclerosis, peripheral artery disease or claudication
Complications
Claudication is generally considered a warning of significant atherosclerosis in the circulatory system, indicating an increased risk of heart attack or stroke. Additional complications of peripheral artery disease due to atherosclerosis include:
- Skin lesions that don’t heal
- Death of muscle and skin tissues (gangrene)
- Amputation of a limb
Treatment
The goals of treating claudication and peripheral artery disease are to reduce pain and manage the risk factors that contribute to vascular disease.
Exercise
Exercise reduces pain, increases exercise duration, improves vascular health in the affected limbs, and contributes to weight management and an overall improvement in your quality of life.
Recommended walking programs include:
- Walking until you feel moderate pain
- Resting to relieve pain
- Walking again
- Repeating the walk-rest-walk cycle for 30 to 45 minutes
- Walking three or more days a week
Supervised exercise is recommended for beginning the treatment, but long-term exercise at home is important for ongoing disease management.
At Alimran Medical Center, we may recommend any of the following treatments
Regenerative medicine treatment (Prolotherapy)
Neurons stimulation
Repetitive Transcranial Magnetic Stimulation, rTMS
Transcranial direct current stimulation (tDCS)
- Electrical stimulation
- Short and long wave
- Laser therapy
- Ultrasonic therapy
- Magnatic therapy
- Exercises
Chiropractic
